Last Updated on July 20, 2022
Overview
Diabetic neuropathy or Diabetic Nerve Pain is nerve damage that can occur if you have diabetes. High blood sugar (glucose) can injure nerves throughout the body. Diabetic peripheral neuropathy is the most typical form of diabetic neuropathy. The hands and arms are the next to be affected, then the feet and legs. The condition typically takes years or even decades to fully manifest.
Pain, tingling, numbness, or weakness in your hands or feet are typical initial signs and symptoms of peripheral neuropathy. If your peripheral neuropathy is severe or has persisted for a while, you could be more susceptible to wounds or infections.
Continue reading the blog to know more about Diabetic Nerve Pain symptoms, risk factors, complications, and how to overcome them.
Diabetic Nerve Pain Symptoms
The following are some symptoms of peripheral neuropathy:
- Numbness, tingling, and burning feelings starting in the toes and fingers and spreading up the legs or arms
- Loss of muscle strength in the hands and feet
- Not being able to sense pain, heat, or cold
- Decline in balance
- Charcot’s joint (joint disintegrates due to nerve problems, frequently in the feet)
- Challenging to walk and find balance
The inability to feel pain, heat or cold can cause new issues. For instance, a foot blister that did not cause pain, in the beginning, may develop into an ulcer. Gangrene may form as the infection progresses and further worsens the Diabetic Nerve Pain symptoms.
Risk factors
 Anyone with diabetes is susceptible to neuropathy. But these significant risk factors raise the possibility of nerve damage:
Anyone with diabetes is susceptible to neuropathy. But these significant risk factors raise the possibility of nerve damage:
Poor control of blood sugar:
Every diabetes complication, including nerve damage, is made more likely by uncontrolled blood sugar.
History of diabetes:
The longer a person has diabetes, especially if blood sugar isn’t well controlled, the greater the risk of developing diabetic neuropathy.
Kidney diseases:
Kidney damage is a risk with diabetes. Toxins enter the bloodstream when the kidneys are damaged, which can cause nerve damage.
Obesity:
A body mass index (BMI) of 25 or higher is associated with an increased risk of diabetic neuropathy.
Smoking:
Smoking causes the arteries to narrow and harden, which reduces blood flow to the legs and feet. This harms the peripheral nerves and makes it more difficult for wounds to heal.
Complications
Several severe complications brought on by Diabetic Nerve Pain include:
Hypoglycemia Unawareness:
Shaking, perspiration, and a rapid heartbeat are typical symptoms of low blood sugar, which is defined as 3.9 millimoles per liter (mmol/L) or less than 70 milligrams per deciliter (mg/dL). However, those who have autonomic neuropathy might not notice these symptoms.
Loss of a foot, leg, or toe:
Even small cuts can develop into sores or ulcers without being noticed if there is nerve damage, which can lead to a loss of feeling in the feet. In extreme circumstances, an infection can destroy tissue or spread to the bone. It might be necessary to amputate a toe, a foot, or even a portion of a leg.
Urinary incontinence and urinary tract infections:
The bladder may not empty completely when urinating if the nerves that control it are damaged. Urinary tract infections can be brought on by bacteria that can accumulate in the bladder and kidneys. The ability to feel the urge to urinate or to control the muscles that release urine can both be affected by nerve damage, which can result in leakage (incontinence).
Sudden blood pressure drop:
The body’s capacity to regulate blood pressure can be impacted by damage to the nerves that control blood flow. Standing up after sitting or lying down can result in a sudden drop in blood pressure, which increases the risk of dizziness and fainting.
Digestive problems:
Digestive issues constipation, diarrhea, or both may occur if the digestive tract’s nerves are damaged.
Gastroparesis:
A condition in which the stomach empties too slowly or not at all, can result from diabetes-related nerve damage. Indigestion and bloating may result from this.
Increased or decreased sweating:
Nerve damage can interfere with sweat gland function, making it more difficult for the body to regulate its temperature.
Prevention
By closely controlling your blood sugar and taking good care of your feet, you can prevent or delay Diabetic Nerve Pain and its complications.
Blood sugar control
The American Diabetes Association (ADA) advises people with diabetes to get an A1C (glycated hemoglobin) test at least twice a year. Your average blood sugar level over the previous two to three months is determined by this test.
Although individual A1C targets may be necessary, the ADA suggests an A1C of less than 7.0% for many adults. If your blood sugar levels exceed your target, you may need to make changes to how you manage your daily activities, such as adding or adjusting medications, changing your diet, or increasing your physical activity. Controlling your blood sugar levels is the key to reducing your Diabetic Nerve Pain symptoms.
Foot care
DPN frequently leads to foot issues, such as sores that never heal, ulcers, and even amputation. But by getting a thorough foot exam at least once a year, you can avoid many of these issues. Additionally, ask your doctor to examine your feet each time you visit and take good care of your feet at home.
Pay attention to your doctor’s advice regarding proper foot care. To safeguard the well-being of your feet:
- Every day, check your feet. Look for redness, swelling, skin that is peeling or cracked, blisters, cuts, and bruises. To check the areas of your feet that are difficult to see, use a mirror or enlist the assistance of a friend or family member.
- Keep your feet dry and spotless. With lukewarm water and mild soap, wash your feet every day. Don’t let your feet soak. Completely dry your feet, including in-between your toes.
- Put lotion on your feet. This lessens the risk of cracking. However, avoid applying lotion between your toes as this could promote fungus growth.
- Carefully trim your toenails. Your toenails should be squared off. To achieve smooth edges, carefully file the edges. A podiatrist, who specializes in foot issues, can assist if you are unable to do this on your own.
- Put on fresh, dry socks. Choose cotton or moisture-wicking fibers for your socks, and avoid those with tight bands or thick seams.
- Wear comfortable, cushioned shoes. To protect your feet, put on closed-toe footwear or slippers.
- Make sure your shoes are comfortable and give you room to move your toes. A foot expert can instruct you on how to select shoes that fit correctly and how to avoid issues like corns and calluses.
Diagnosis
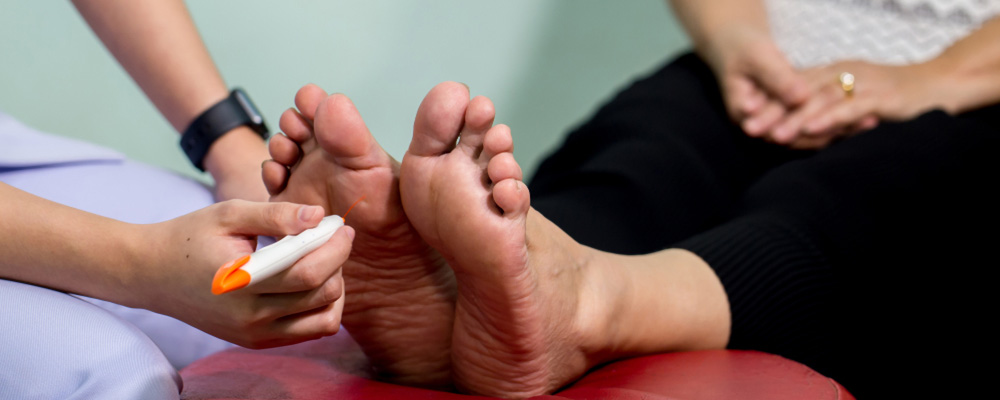 Typically, Diabetic Nerve Pain can be identified by a physical examination, a careful review of your diabetic peripheral neuropathy symptoms, and medical history.
Typically, Diabetic Nerve Pain can be identified by a physical examination, a careful review of your diabetic peripheral neuropathy symptoms, and medical history.
Usually, your physician examines:
- overall muscle tone and strength
- tendon reactions
- sensitivity to pain, temperature, vibration, and touch
Your doctor may ask for the following tests in addition to the physical examination to help diagnose diabetic neuropathy:
Filament testing:
Your skin is brushed with a smooth nylon fiber (monofilament) to gauge how sensitive you are to touch.
Sensory evaluation:
This painless test determines how your nerves react to vibration and temperature changes.
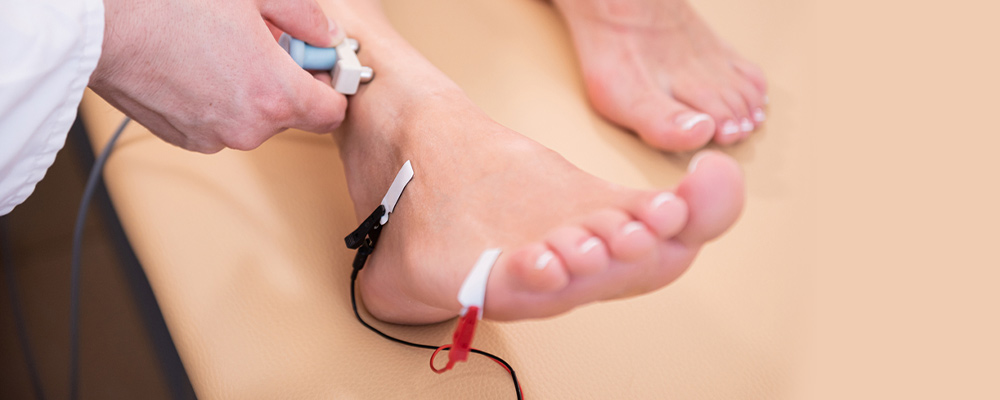
Testing nerve conduction:
This examination evaluates how quickly your arms and legs’ nerves transmit electrical signals.
Electromyography:
This test, also known as needle testing, is frequently perform along with nerve conduction studies. It counts the electrical impulses that leave your muscles.
 Autonomic evaluation:
Autonomic evaluation:
It may be necessary to undergo specific tests to check your sweating and how your blood pressure changes when you are in various positions.
Treatment
There is no cure for diabetic peripheral neuropathy symptoms. However, treatment of diabetic nerve pain symptoms can improve the quality of life. The objectives of treatment include:
- Slow progression
- Relieve pain
- Manage complications and restore function
Slowing the disease’s progression
The key to avoiding or postponing nerve damage is maintaining your blood sugar levels consistently within your target range. Maintaining healthy blood sugar levels might even help some of your present symptoms. Based on your age, the duration of your diabetes, and your general health, your physician will determine your ideal target range.
Individual blood sugar levels must be monitored. However, for the majority of diabetics, The American Diabetes Association (ADA) suggests the following target blood sugar levels:

- Before meals, between 4.4 and 7.2 mmol/L (80 to 130 mg/dL).
- Two hours after meals, less than 180 mg/dL (10.0 mmol/L).
For the majority of diabetics, the ADA suggests an A1C of 7.0% or lower.
Keeping your blood pressure under control, maintaining a healthy weight, and engaging in regular physical activity are additional crucial ways to help slow or prevent neuropathy from getting worse.
Relieving pain
Numerous prescription drugs can treat nerve pain which is one of Diabetic Nerve Pain symptoms, but not everyone finds success with them. Talk to your doctor about the advantages and potential side effects of any medications you’re thinking about taking to determine which one would be most effective for you. Prescription remedies for pain management could consist of:
Anti-seizure drugs:
Some drugs that are used to treat epilepsy also help to relieve nerve pain. The ADA advises pregabalin as a starting point (Lyrica). Another choice is gabapentin (Gralise, Neurontin). Drowsiness, vertigo, and swelling in the hands and feet are possible side effects.
Antidepressants:
Even if you are not depressed, some antidepressants can relieve nerve pain. Mild to moderate nerve pain may be relieve with tricyclic antidepressants. Amitriptyline, nortriptyline (Pamelor), and desipramine are medications in this class (Norpramin). Dry mouth, constipation, drowsiness, and difficulty concentrating are some unwelcome side effects. When changing positions, such as from lying down to standing, these medications may also make you feel lightheaded (orthostatic hypotension).
SNRIs (Serotonin and norepinephrine reuptake inhibitors), a different class of antidepressants with fewer side effects that may help with nerve pain, are serotonin and norepinephrine reuptake inhibitors. Duloxetine (Cymbalta, Dreama Sprinkle) is suggested by the ADA as the initial therapy. Venlafaxine is another that could be utilize (Effexor XR). Nausea, sleepiness, vertigo, decreased appetite, and constipation are examples of potential side effects.
An antidepressant and a seizure medication may occasionally be taken together. These drugs can also be combine with painkillers, such as those that are over-the-counter. Acetaminophen (Tylenol, among others), ibuprofen (Advil, Motrin IB, among others), or a skin patch containing lidocaine, for instance, may provide relief (a numbing substance).
Managing complications and regaining functionality
You may require treatment from various specialists to manage complications. These may include a Cardiologist who can help prevent or treat cardiac complications and a Urologist who specializes in treating urinary tract issues.
Your neuropathy-related complications and the severity of your Diabetic Nerve Pain symptoms will determine the course of treatment you require:
Urinary system issues:
Your doctor might advise stopping or switching medications because some medications have an adverse effect on bladder function. Some bladder issues can be resolved by following a strict urination schedule or urinating at regular intervals (timed urination) while gently pressing the bladder region (below your belly button). Urine removal from a bladder with damaged nerves may require additional procedures, such as self-catheterization.
Digestive issues:
Eating smaller, more frequent meals may help to relieve the mild signs and symptoms of gastroparesis, such as indigestion, belching, nausea, or vomiting. Gastroparesis, diarrhea, constipation, and nausea may be relieved with dietary changes and medications.
Orthostatic hypotension (low blood pressure on standing):
Simple lifestyle adjustments like abstaining from alcohol, drinking plenty of water, and slowly rising from a sitting position are the first step in treatment. Overnight high blood pressure can be avoid by sleeping with the head of the bed raised by 4 to 6 inches.
Additionally, your doctor might advise that you wear compression sleeves on your thighs and abdomen (abdominal binder and compression shorts or stockings). To treat orthostatic hypotension, several drugs may be use, either separately or in combination.
Bottomline
Diabetes patients with peripheral neuropathy experience dysfunction and damage to their peripheral nerves. DPN can present clinically as nothing or as severe neuropathic pain and numbness. It is a common condition that is challenging to treat. Frequently, it goes unreported and untreated. Diabetic Nerve Pain is link to an increased risk of lower limb amputation, mortality, and foot ulcers.
Patients with diabetes should undergo an annual peripheral neuropathy screening to improve outcomes. Based on symptoms, medical history, and physical examination results, a diagnosis of diabetic peripheral neuropathy is frequently suspected. Because a patient’s neuropathy may have an underlying cause other than diabetes, it is crucial to take a variety of conditions into account when making the differential diagnosis. The cornerstones of treatment are glycemic control and pain management, and several drug classes are thought to be successful in treating Diabetic Nerve Pain symptoms.


 Autonomic evaluation:
Autonomic evaluation: